“Don’t Take It Lung—It’s Just a Bronchogram!”
Written by Dr. Michael Lin
Edited by Dr. Joann Hsu
Case Presentation:
71 year old male with pmhx of heart disease of native coronary artery, HLD, HTN, malignant neoplasm of bronchus or lung, presenting to the ED for respiratory distress. Patient is reportedly NPO and wife fed him food and he became acutely short of breath
Physical Exam
(+) tachypneic, (+) hypoxic to 75% on room air, (+) crackles throughout the lung fields
What are our differentials?!
Let’s use Ultrasound to take a look at the lungs~!
Overview of Ultrasound Pulmonary Views
Use curvilinear probe and select EFAST or Lung views
Apply ultrasound gel and have probe marker facing UP.
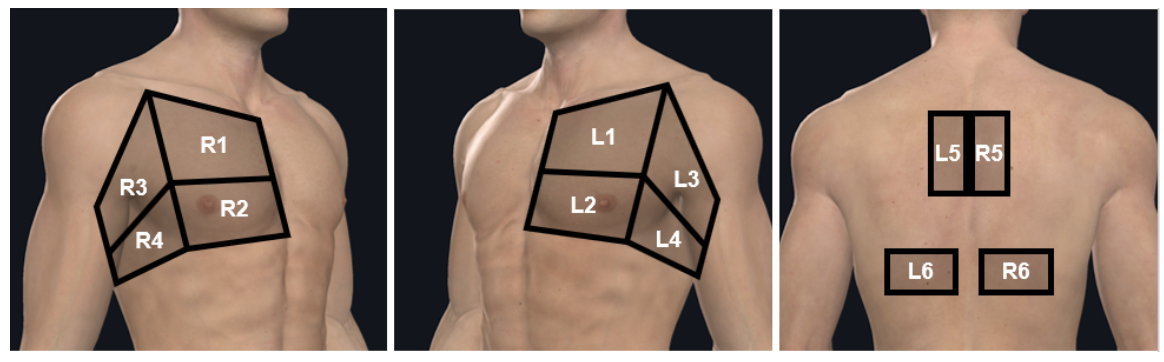
Divide your left and right hemithorax EACH into 4 divisions
Upper Anterior (1): Mid-clavicular line, 2nd-3rd intercostal space (above the nipple line).
Lower Anterior (2): Mid-clavicular line, 4th-5th intercostal space (below the nipple line).
Upper Lateral (3): Anterior axillary line, 3rd-4th intercostal space.
Lower Lateral/Posterior (4 - PLAPS point): Posterior axillary line, 5th-6th intercostal space. Should get the diaphragm into view to assess for pleural effusion. (this is also your Right and Left upper quadrant views on EFAST exam)
Have depth ~15cm. Assess for B-lines, subpleural consolidations, pleural effusion, air bronchograms, masses, etc
How effective is Ultrasound for Pulmonary Pathologies?
Consolidation
Sensitivity 90-98%, specificity 94-98%
Children: Sensitivity 87-89%, specificity 95-100%, positive predictive value 92.5%, negative predictive value 90.8%
Pneumothorax
Superior to supine anterior CXR for ruling in and ruling out PTX
Sensitivity 92-100%, specificity 91-99%, positive predictive value 89-92%, negative predictive value 93-100%
Pleural Effusion
More accurate for diagnosing pleural effusion than supine CXR and nearly as accurate as CT
Sensitivity 88-94%, specificity 96-100%, positive predictive value 92-100, accuracy 90-93%
Can detect as little of 20 mL of fluid,29 whereas upright CXR detects 100-200 mL of fluid
Atelectasis
Sensitivity 82-90%, specificity 89-100%, positive predictive value 84-100%, negative predictive value 86-94%, accuracy 89-91%
Children: Sensitivity 88%, specificity 89%, 88% accuracy
~ so pretty effective!
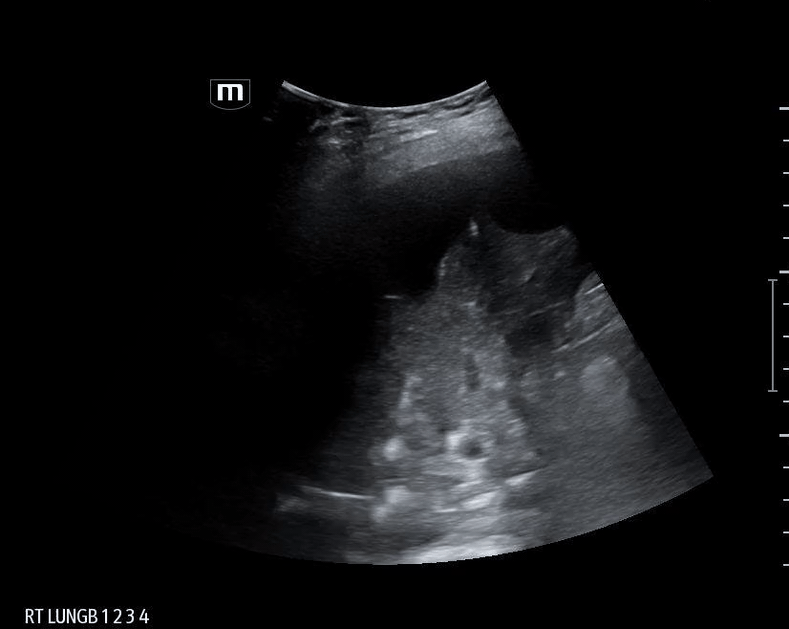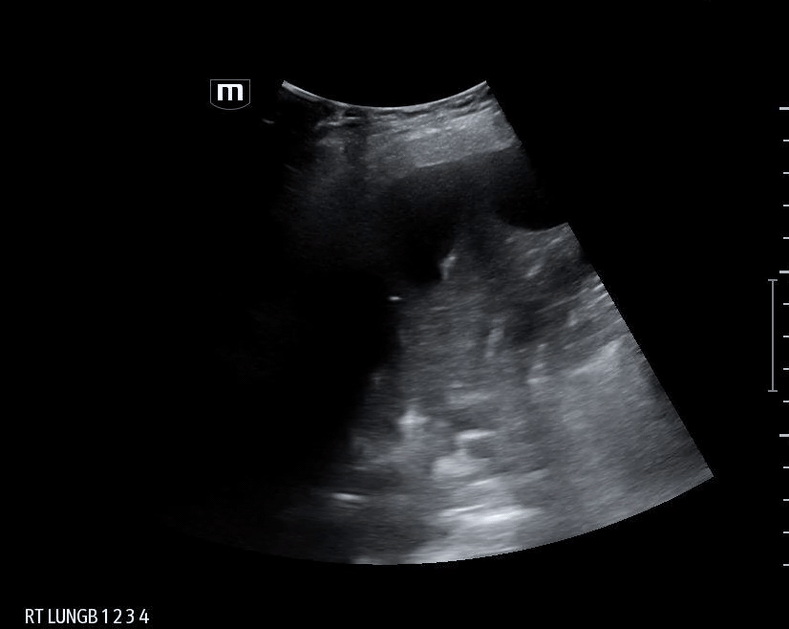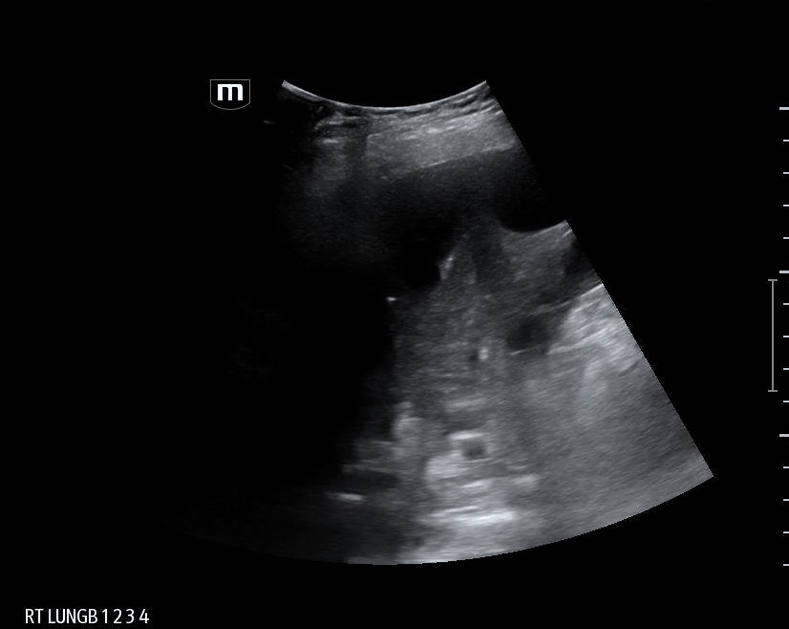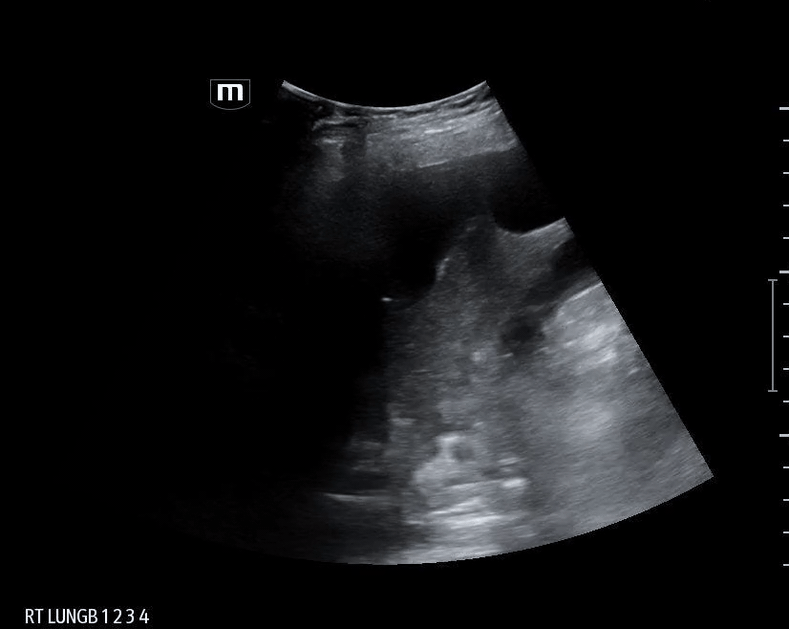
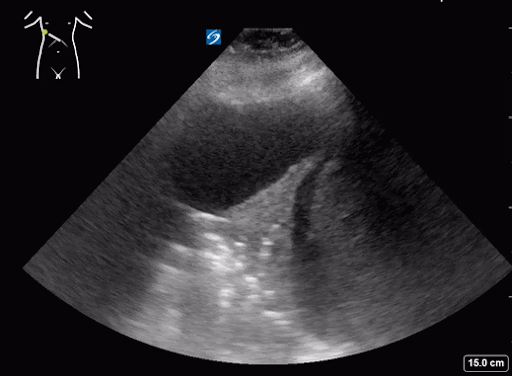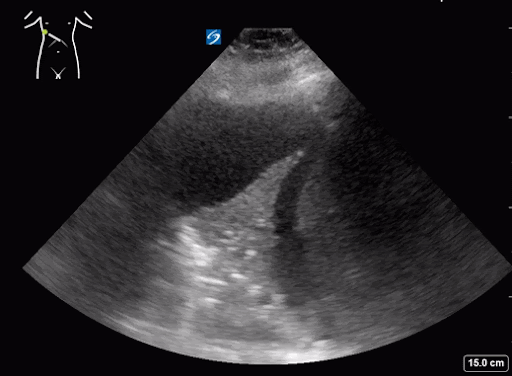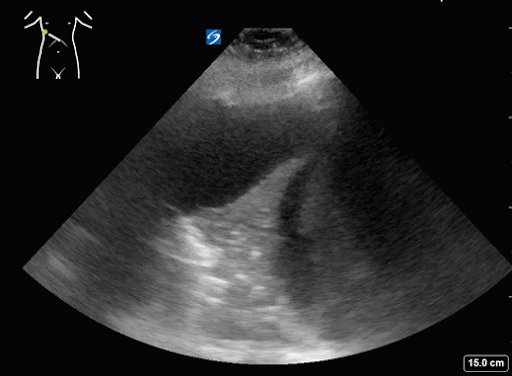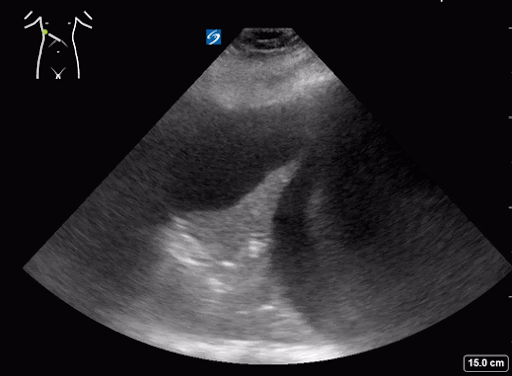
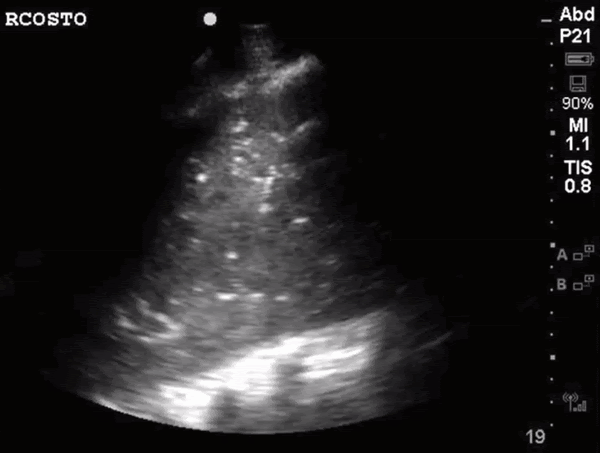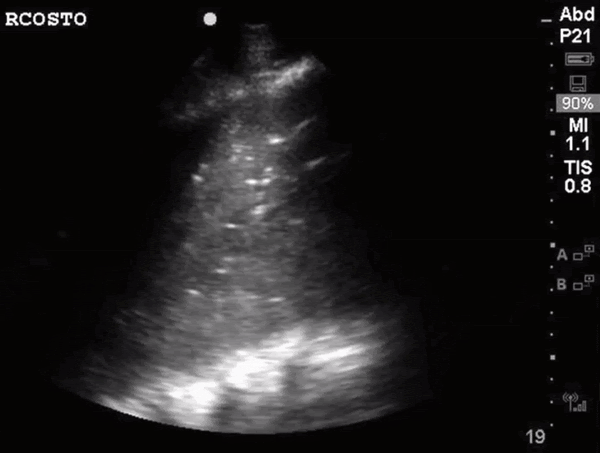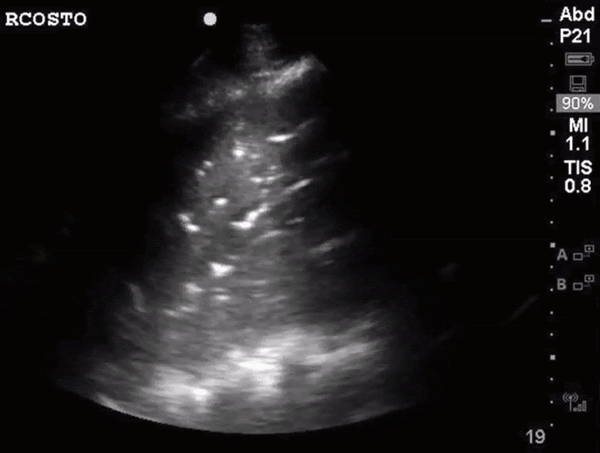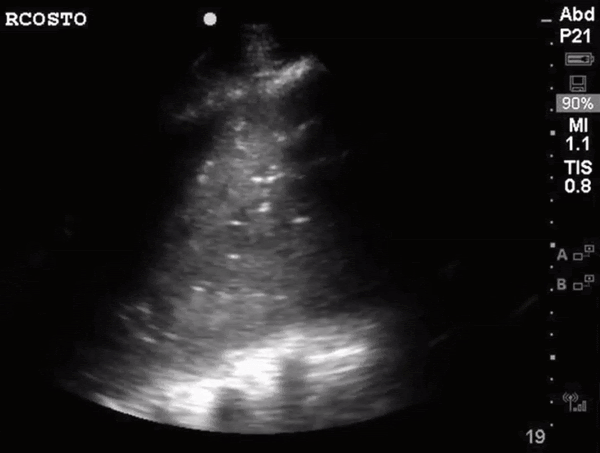
What do we see in this pt’s US?!
Right lung base
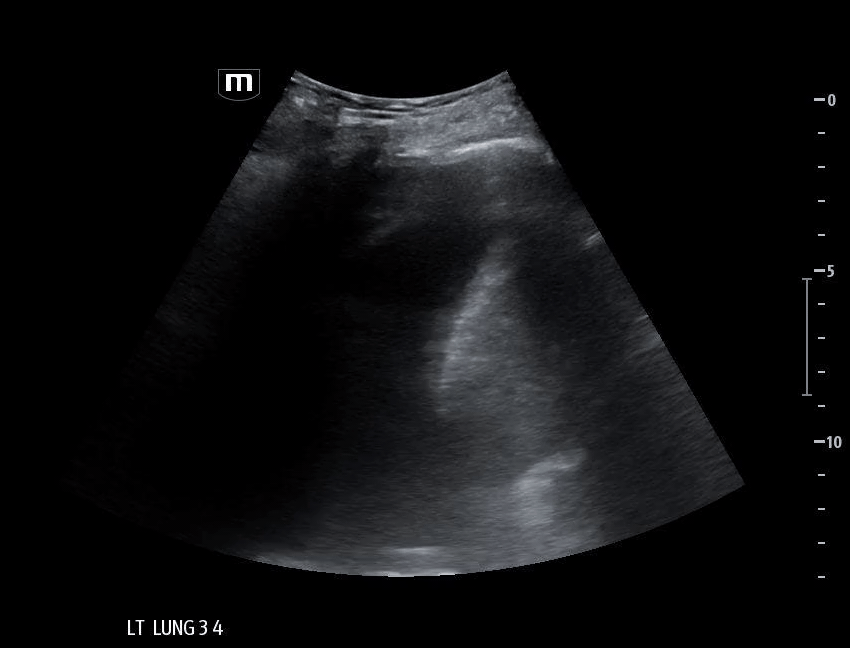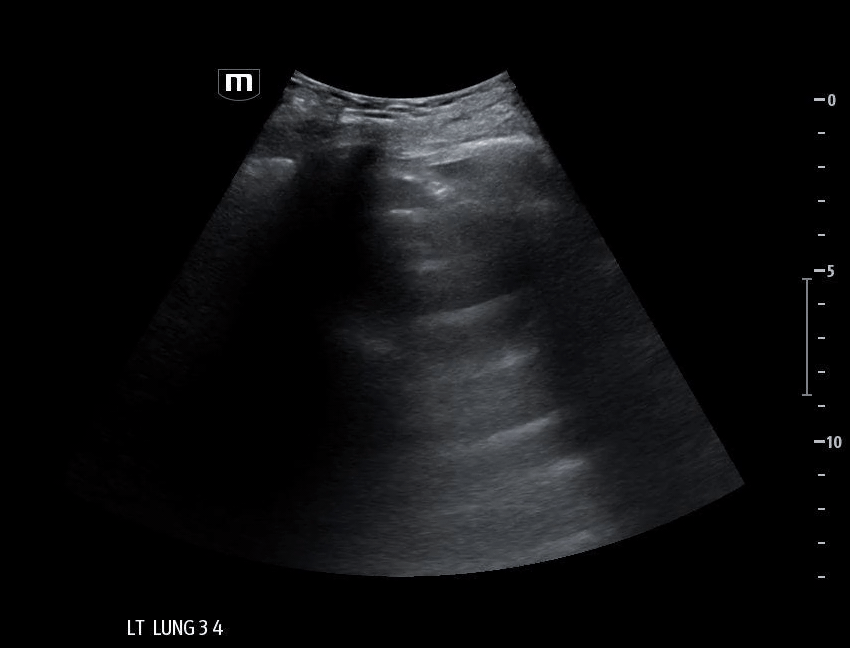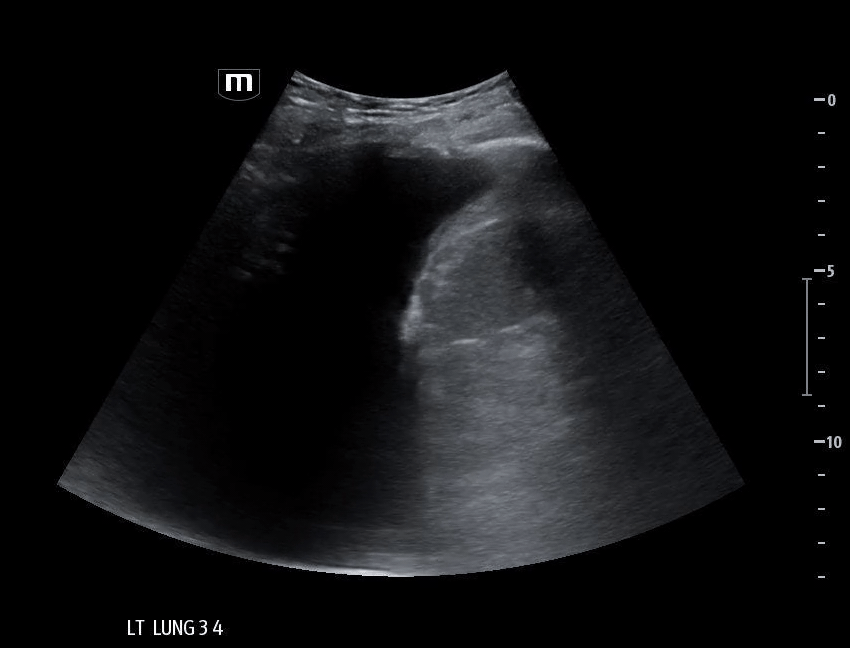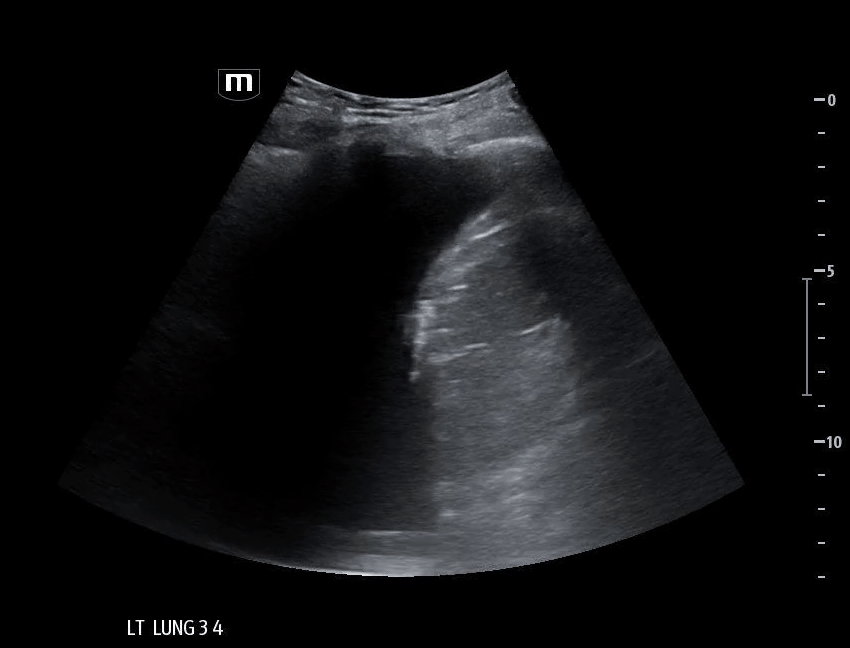
Left lung base
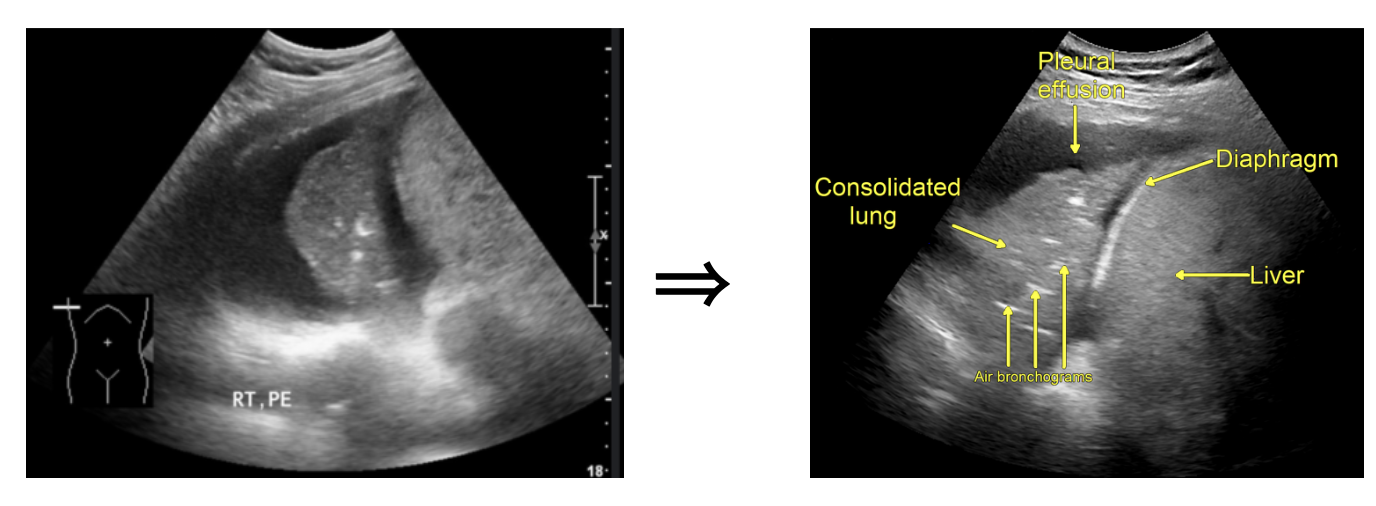
Let’s focus on air bronchograms.
What are they?
Ultrasound is limited in air-rich organs bc air scatters ultrasound waves and cannot transduce them. Hence, typically cannot visualize normal lung tissue but... if there is consolidation and fluid...
Fluid-filled alveoli act as an excellent acoustic medium and allow visualization of the lung parenchyma.
air bronchogram occurs when endobronchial air is visible against a background of increased lung opacity.
Two Types
Static Air Bronchogram
Immobile hyperechoic structure in consolidated or “hepatized” lung → indicating obstructed and trapped air → usually sign of atelectasis
Dynamic Air Bronchogram
Mobile hyperechoic structure in consolidated or “hepatized” lung → indicating patent airway ⇒ pathognomonic for pneumonia
Dynamic air bronchogram had a specificity of 94% and a positive predictive value of 97% for pneumonia.
Ok back to case…
Patient’s CT chest came back positive for right sided aspiration pneumonia and right lung collapse secondary to pleural effusions.
Happy scanning!
Sources
Abhilash Koratala. “Pneumonia and Dynamic Air Bronchograms.” NephroPOCUS, July 2019,nephropocus.com/2019/07/01/dynamic-air-bronchograms-ultrasound-sign-of-pneumonia/.
Alerhand, Steven , and Betul Gulalp. “Sonoguide // Lung.” Acep.org, Sonoguide, 8 Mar. 2021, www.acep.org/sonoguide/basic/lung.
Amini, Behrang, and Stefen Tigges. “Air Bronchogram .” Radiopaedia, 28 Dec. 2025, radiopaedia.org/articles/air-bronchogram?lang=us.
Ashraf A, Air bronchograms on ultrasound. Case study, Radiopaedia.org (Accessed on 20 Mar 2026) https://doi.org/10.53347/rID-159620
Lichtenstein, Daniel, et al. “The Dynamic Air Bronchogram.” Chest, vol. 135, no. 6, June 2009, pp. 1421–1425, https://doi.org/10.1378/chest.08-2281.
Monteiro Pereira Jr, Elmo Fabiano, et al. “Lung Ultrasound in COVID 19 Pandemic. Recommendations - WINFOCUS.” WINFOCUS, Apr. 2020, www.winfocus.org/lung-ultrasound-in-covid-19-pandemic/.