From Zen to Tension: An Acupuncture-Induced Pneumothorax?
Written by: Dr. Quinn Bushman
Edited by: Dr. Joann Hsu
You hear a Trauma Bravo activation called overhead.
A 46-year-old female is rushed into the trauma bay. EMS reports she was found to have a hemothorax on chest radiograph after undergoing acupuncture earlier that day. She is sitting upright on the stretcher, alert but visibly uncomfortable.
Her airway is intact. On auscultation, left-sided breath sounds are present. On the right, however, breath sounds are completely absent.
Vitals are obtained: BP 95/66, HR 95 bpm, SpO₂ 92% on room air, RR 15.
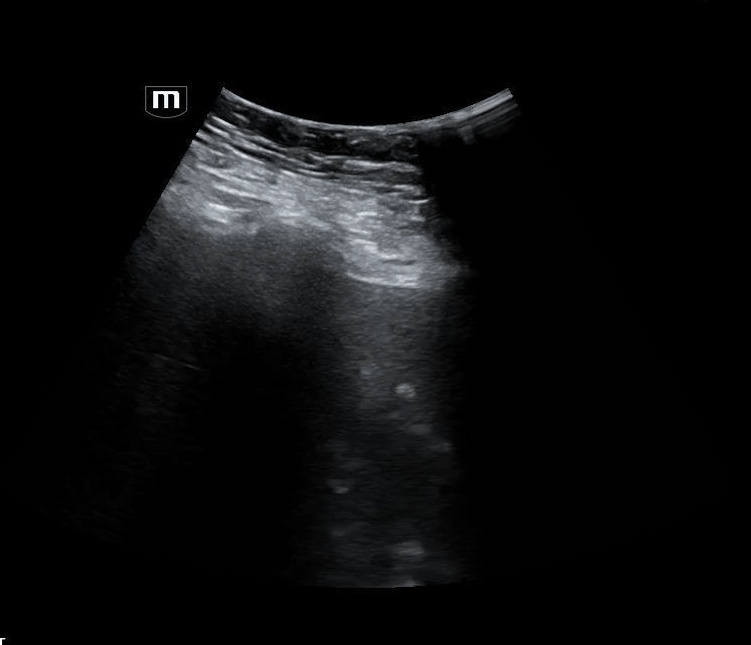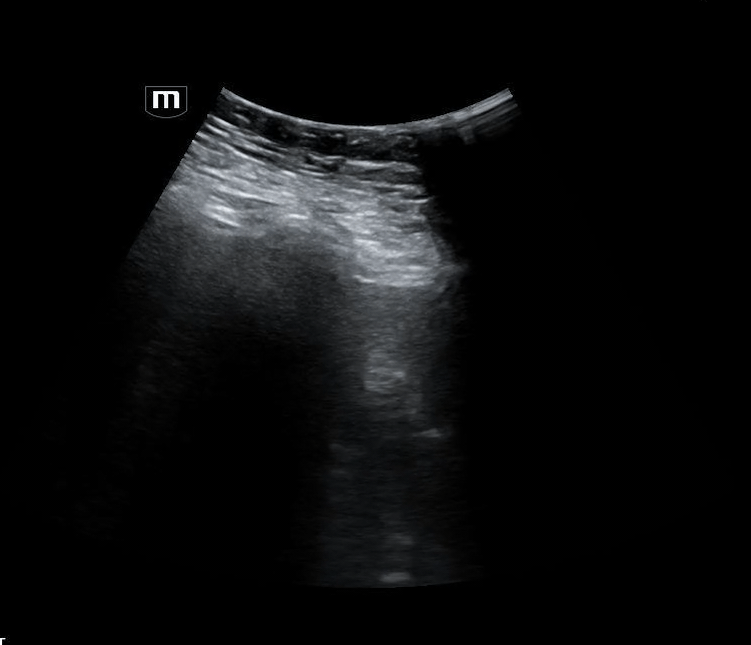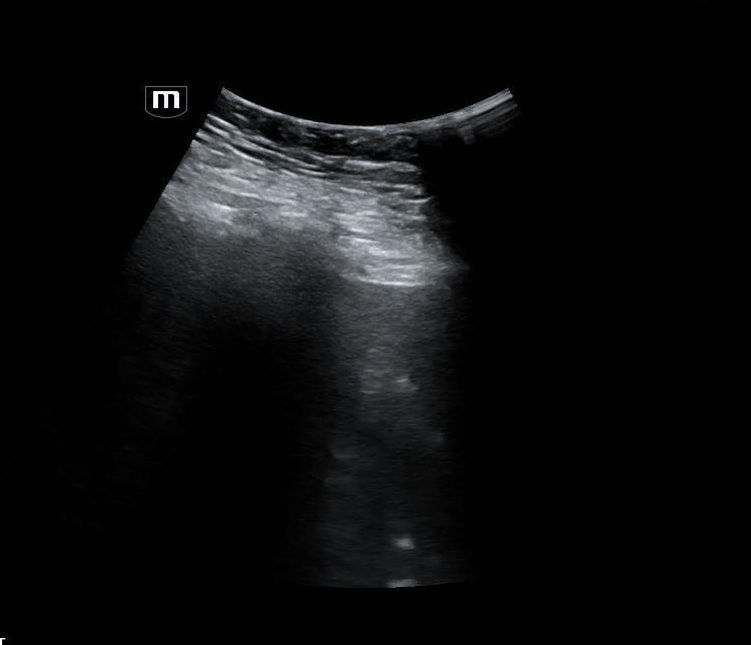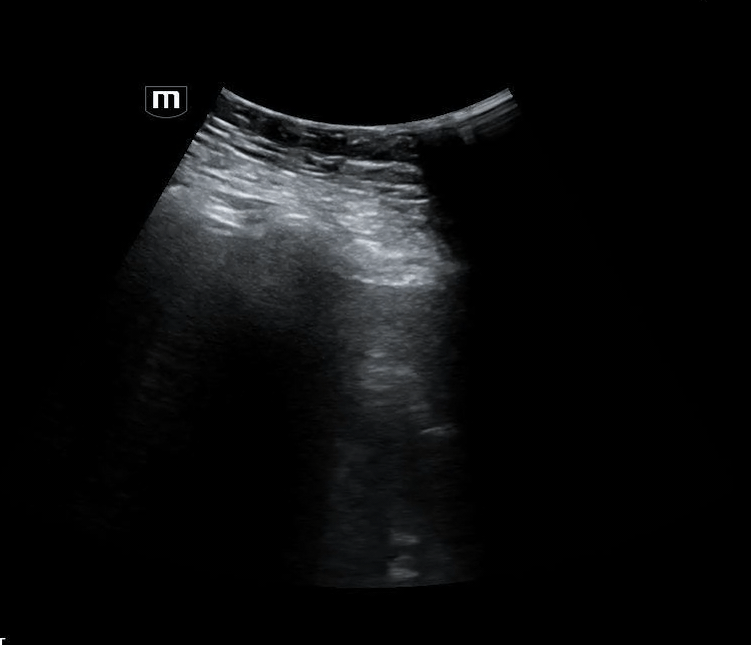
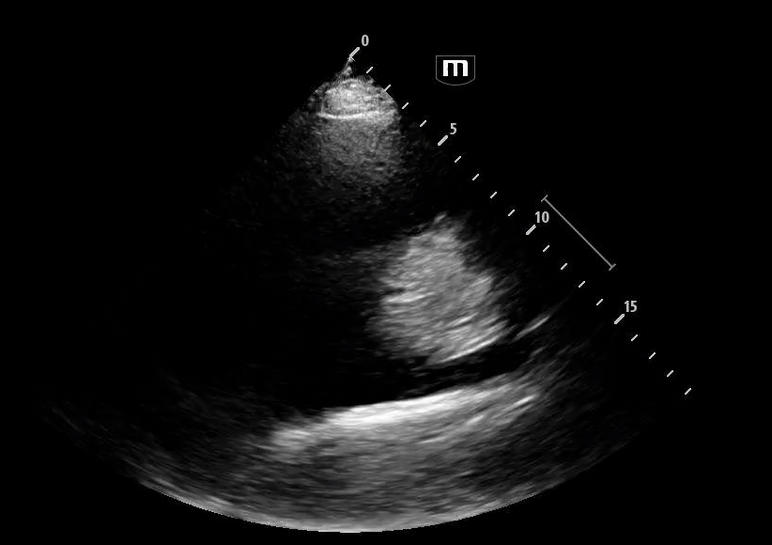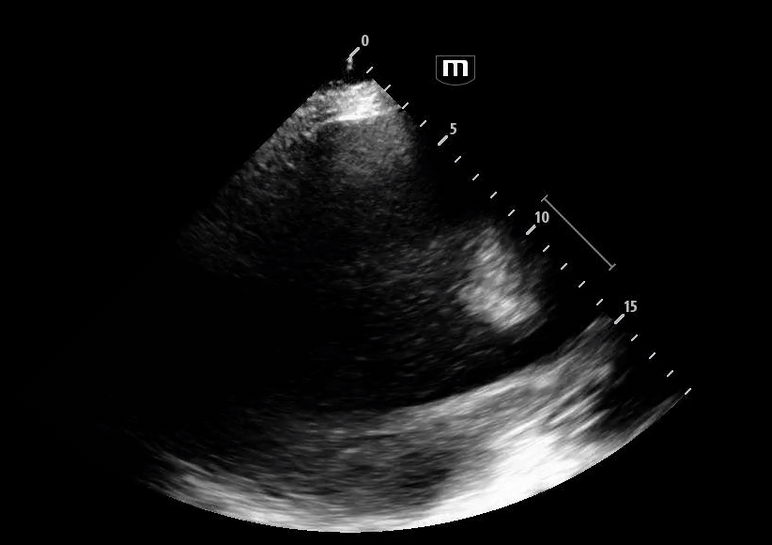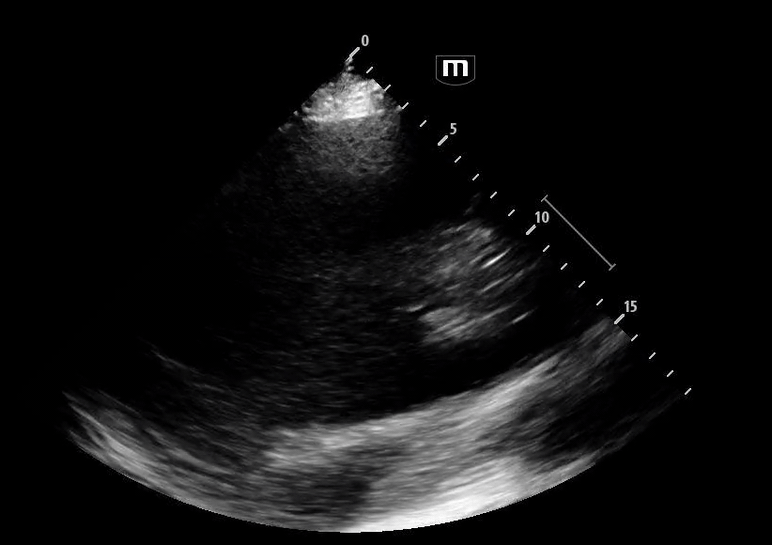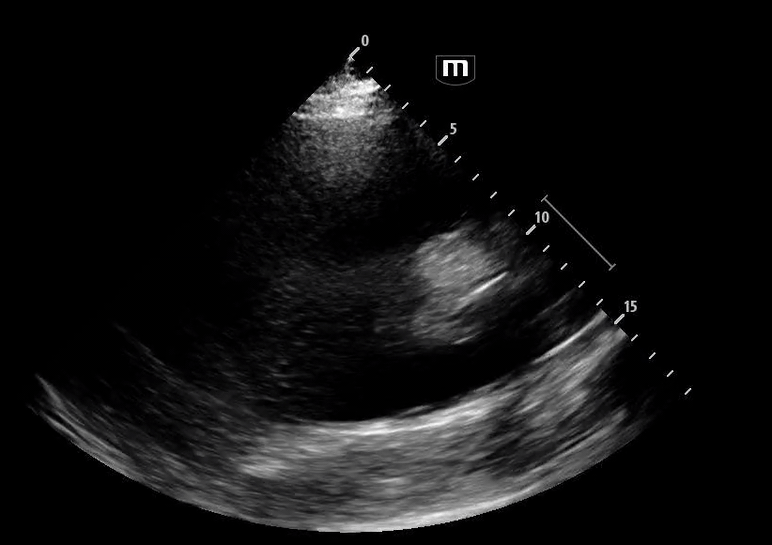
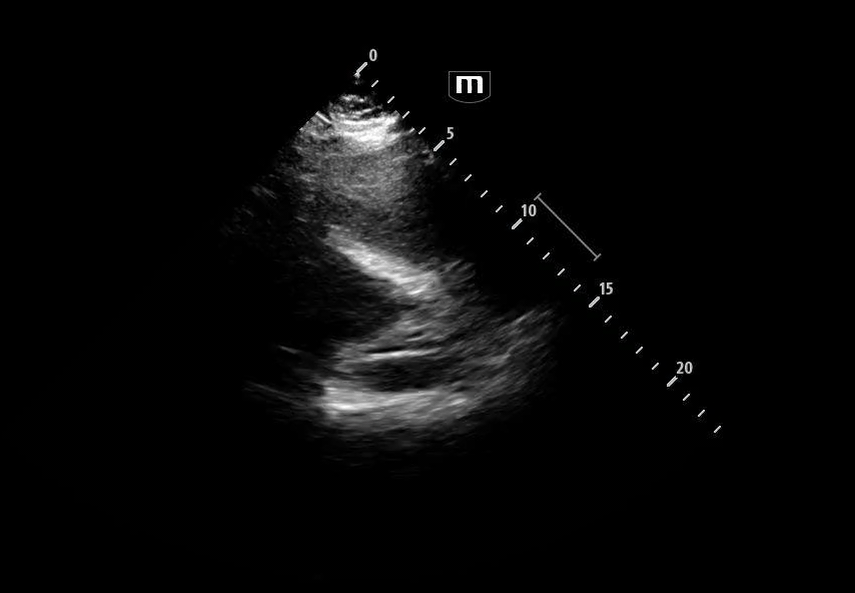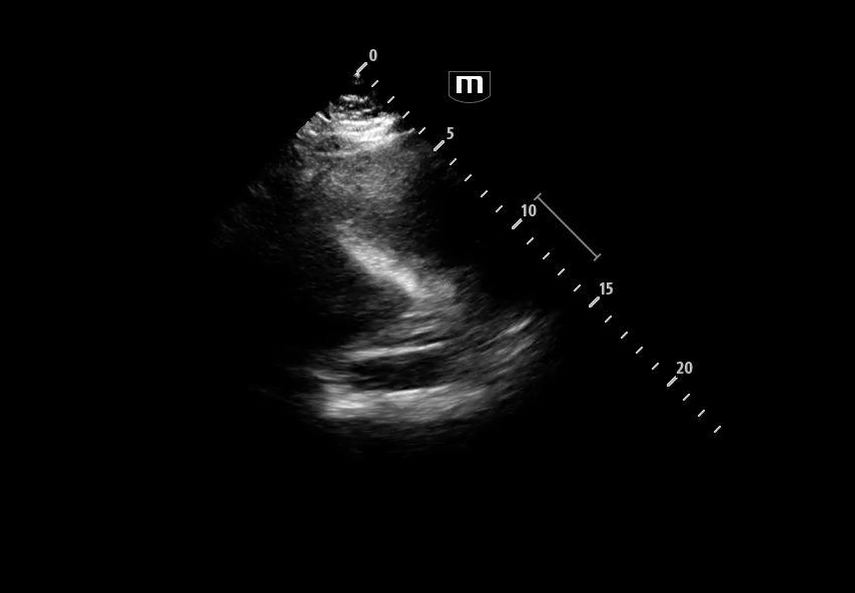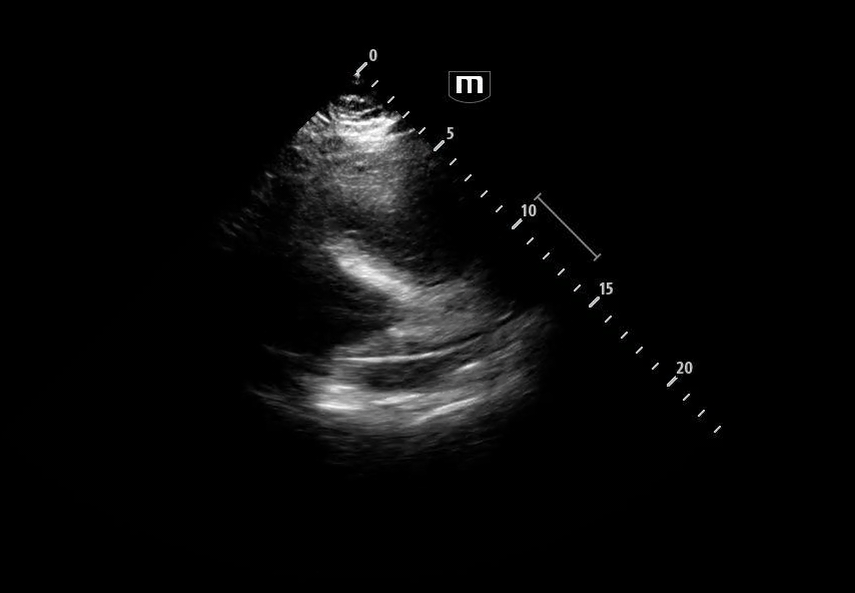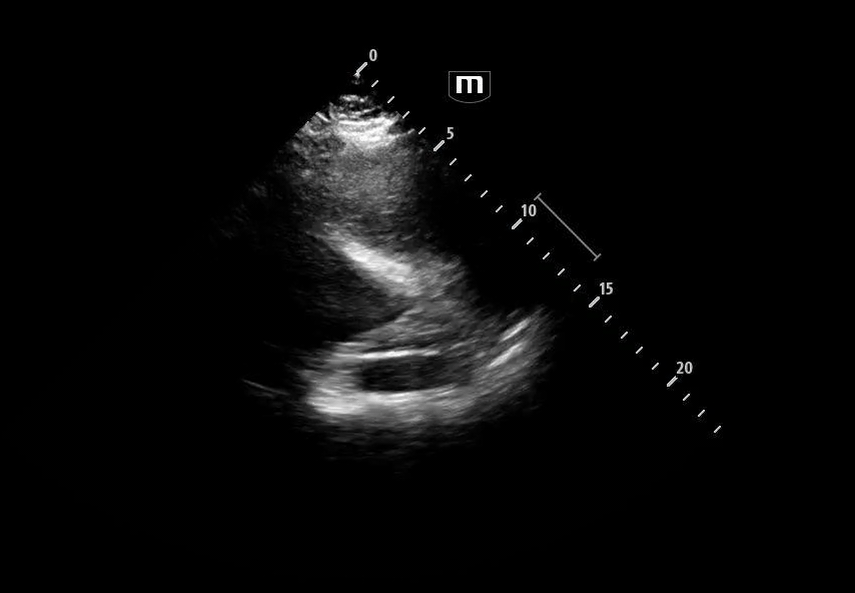
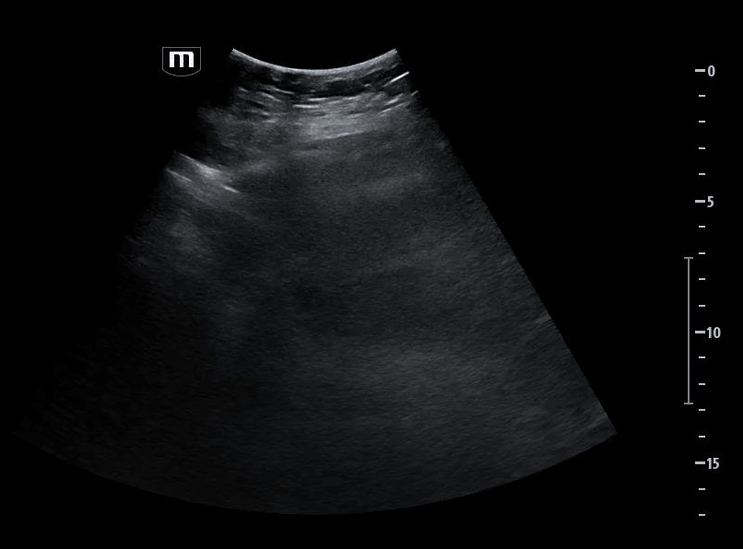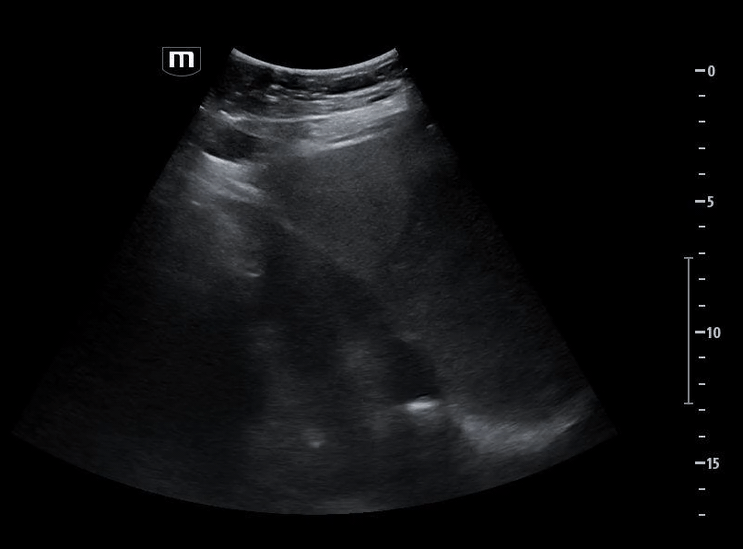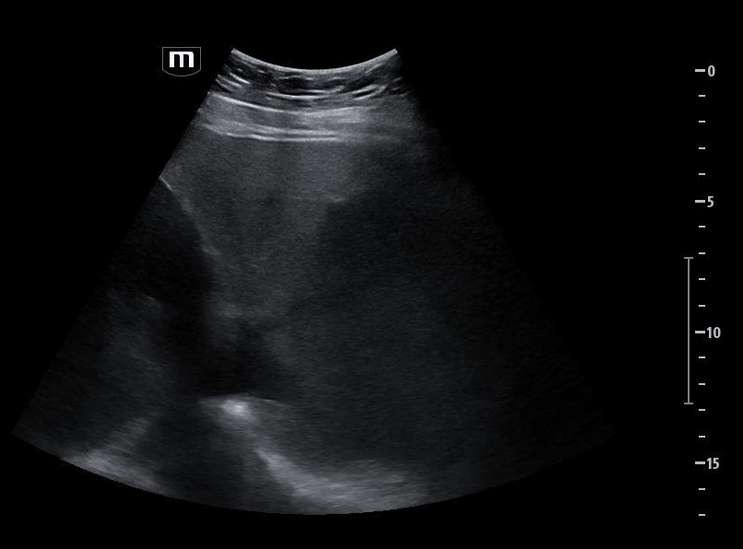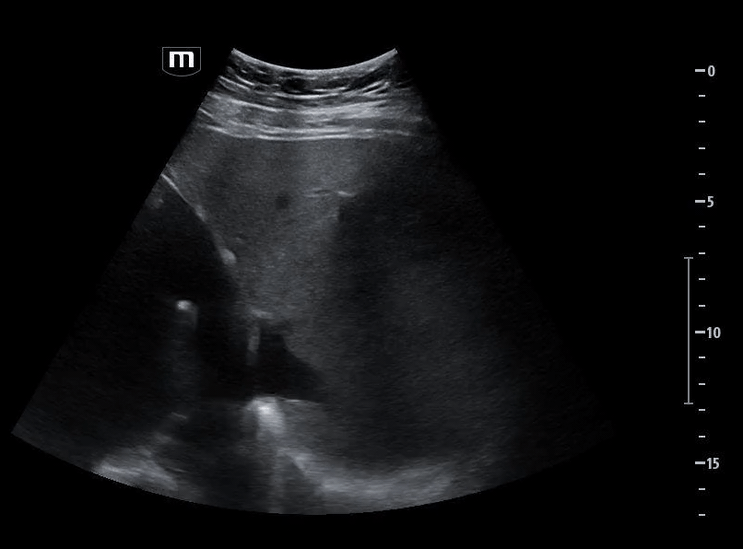
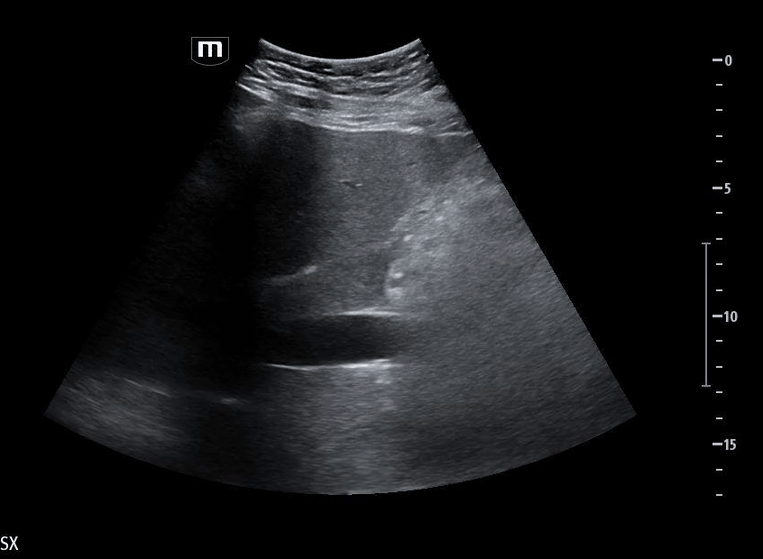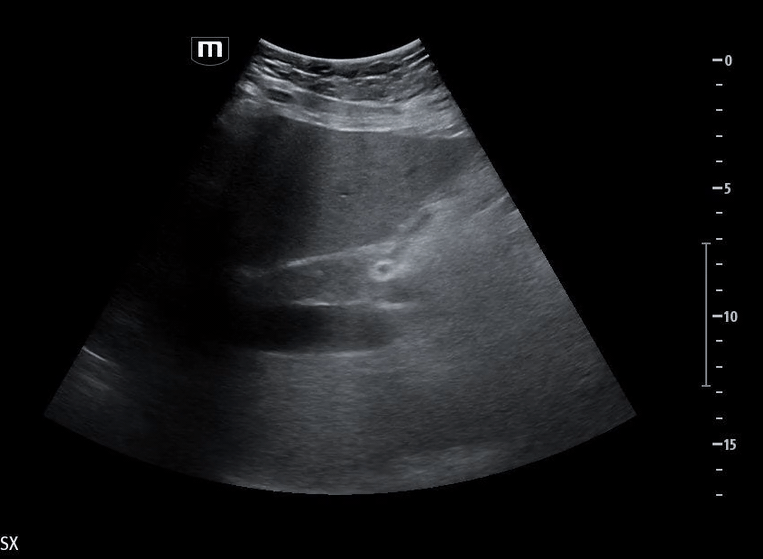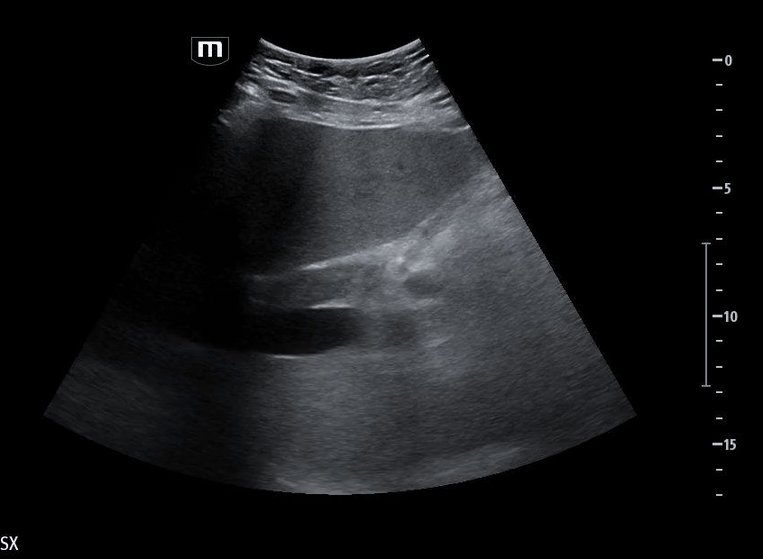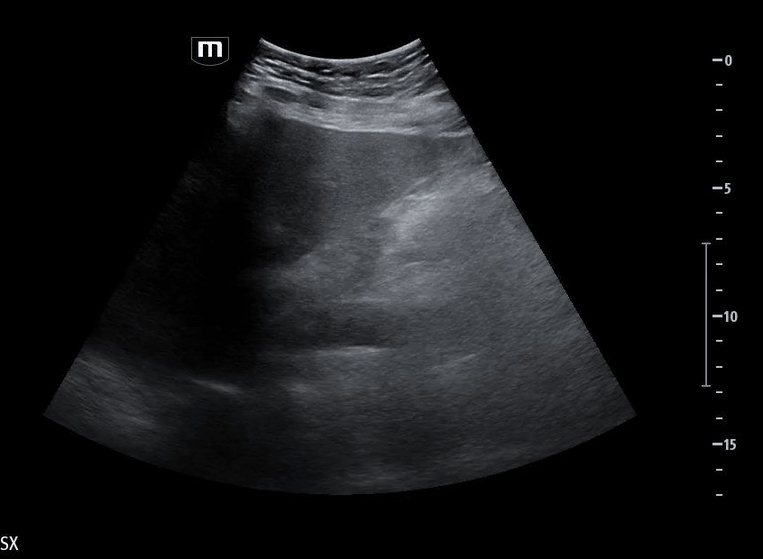
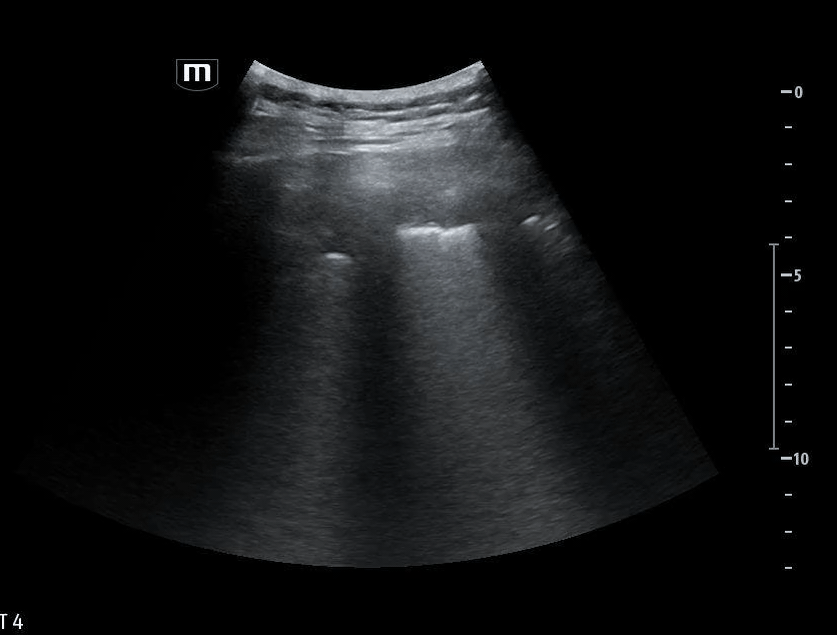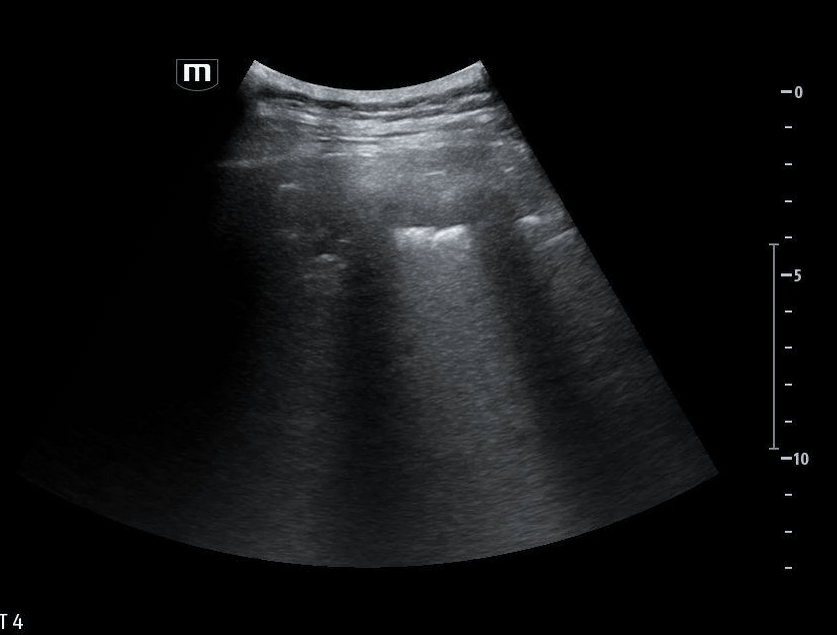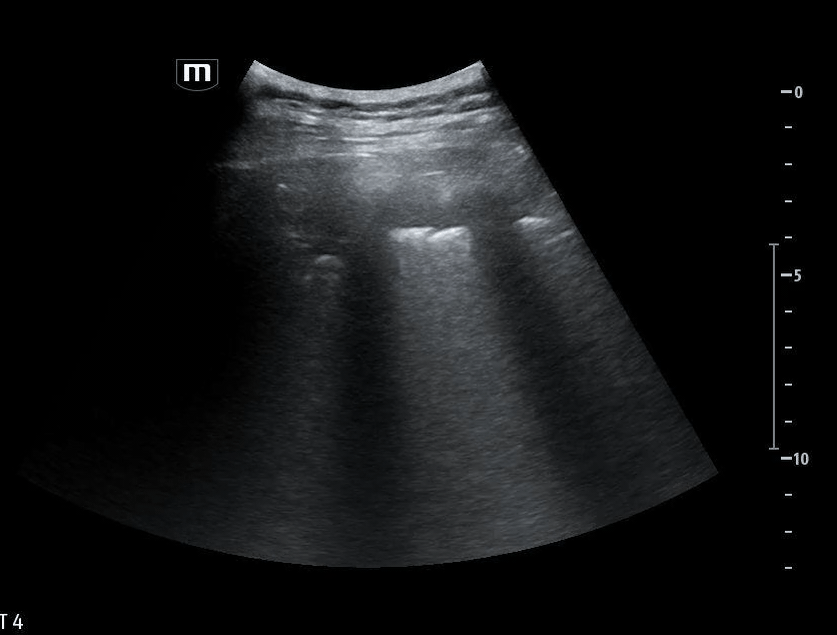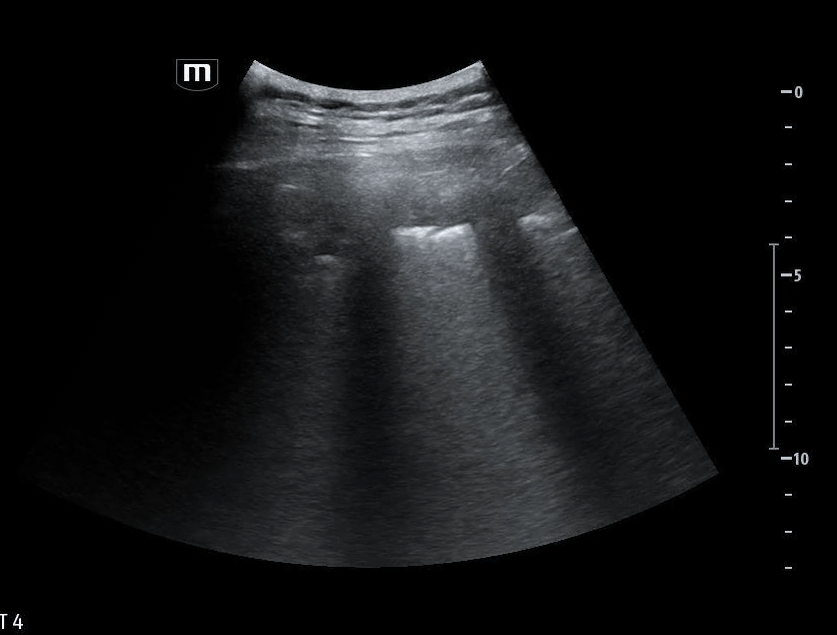
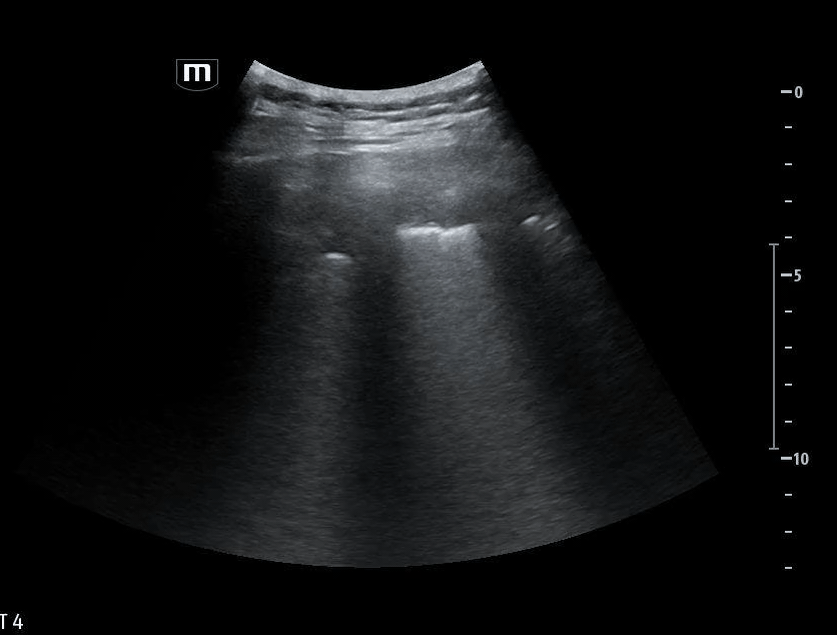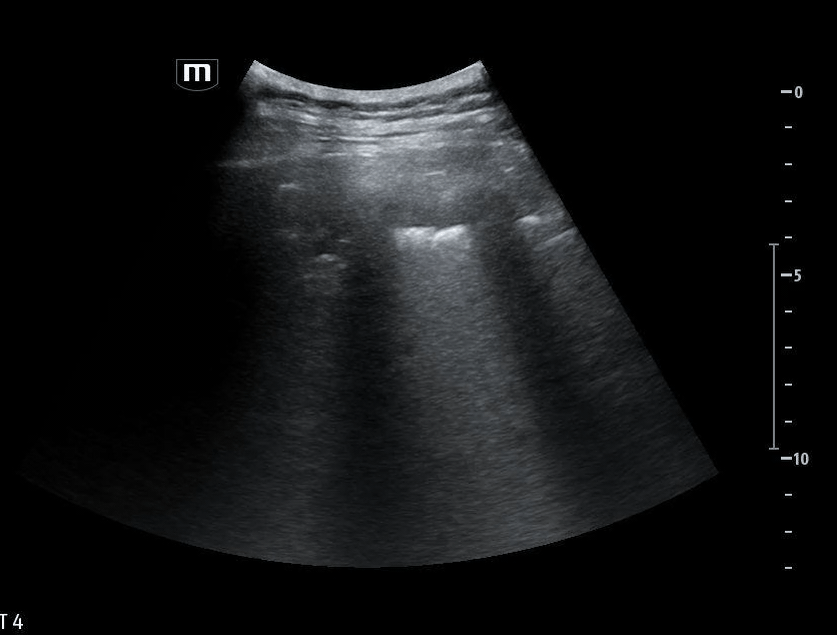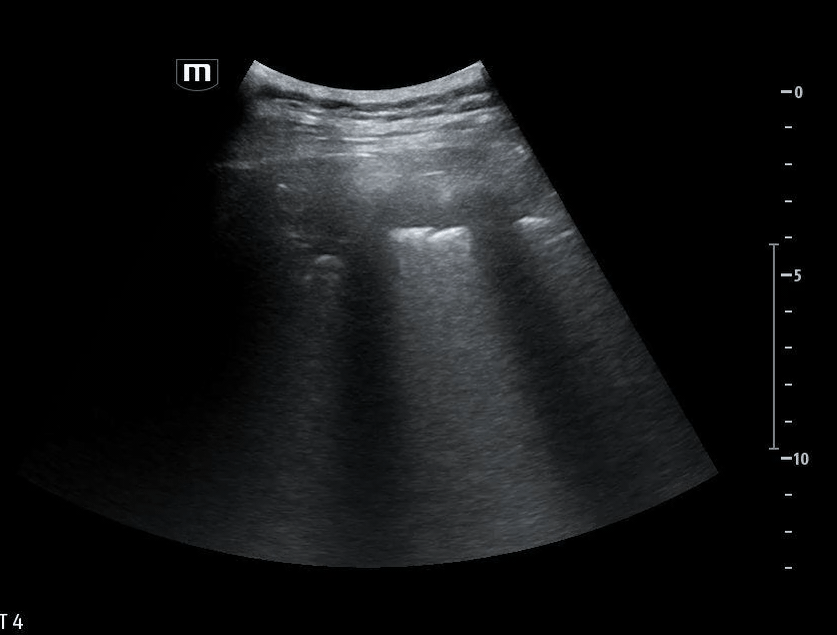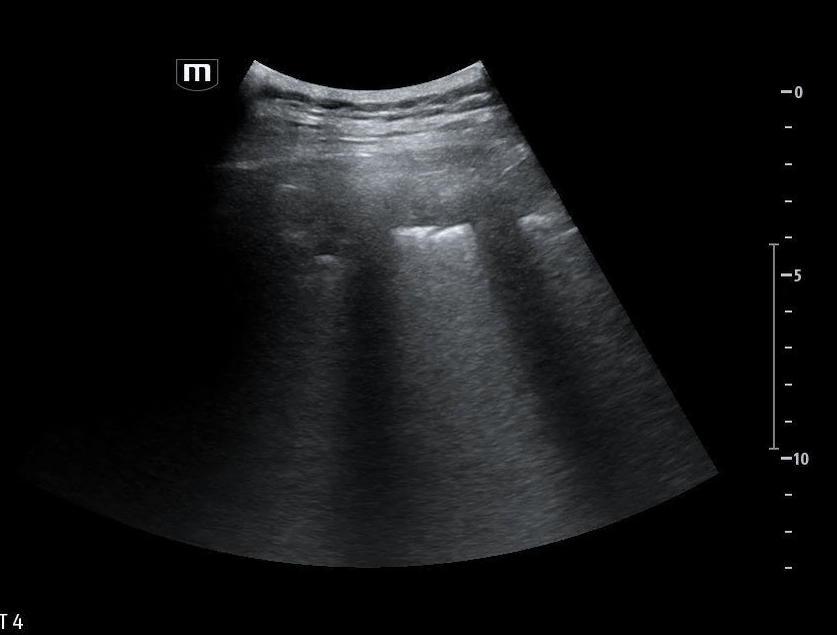
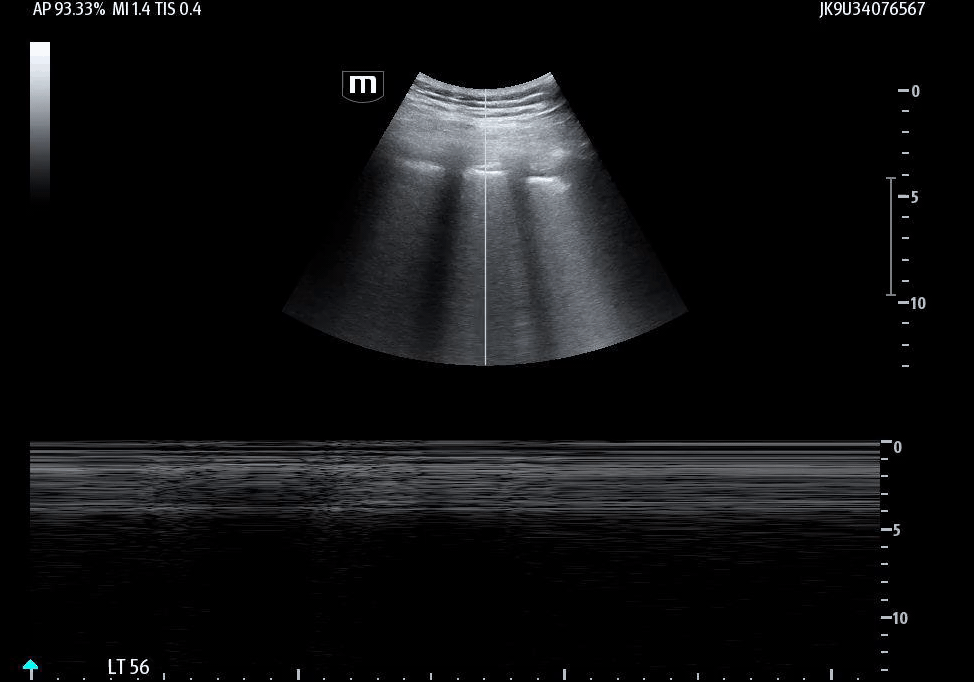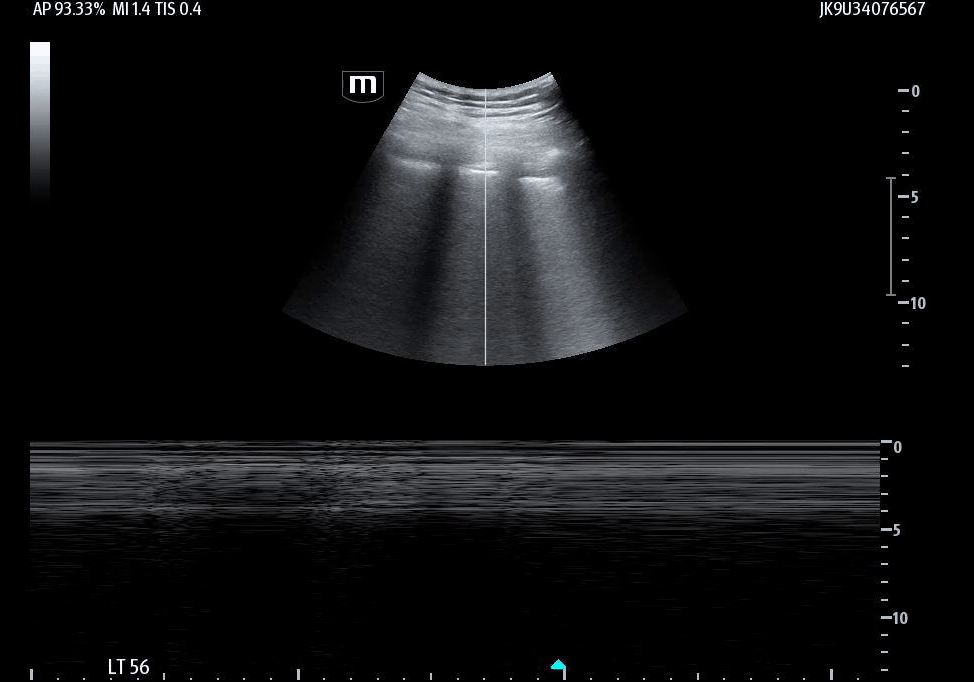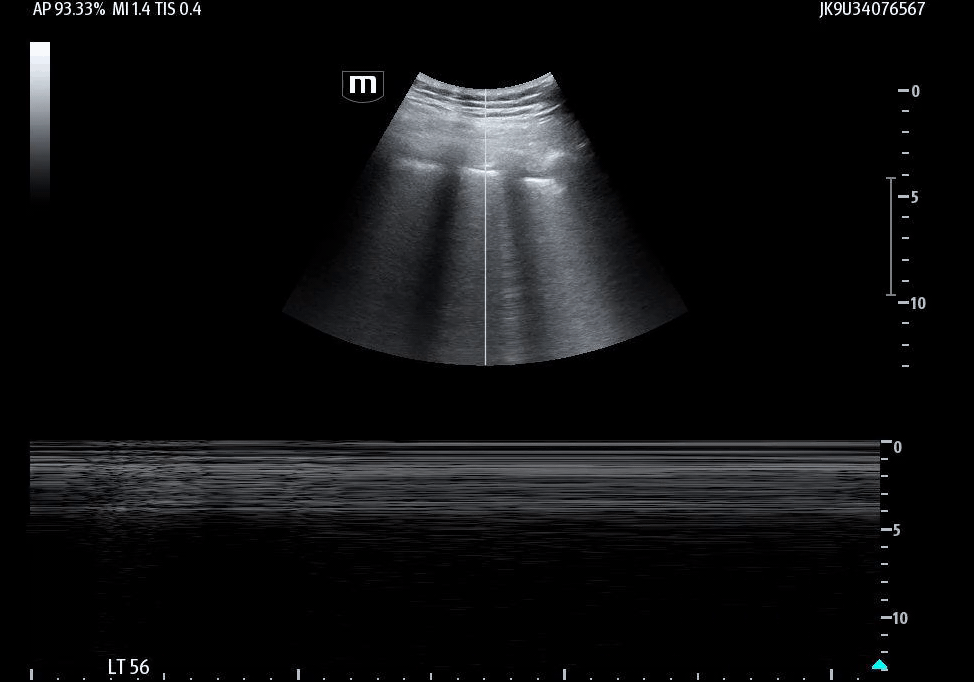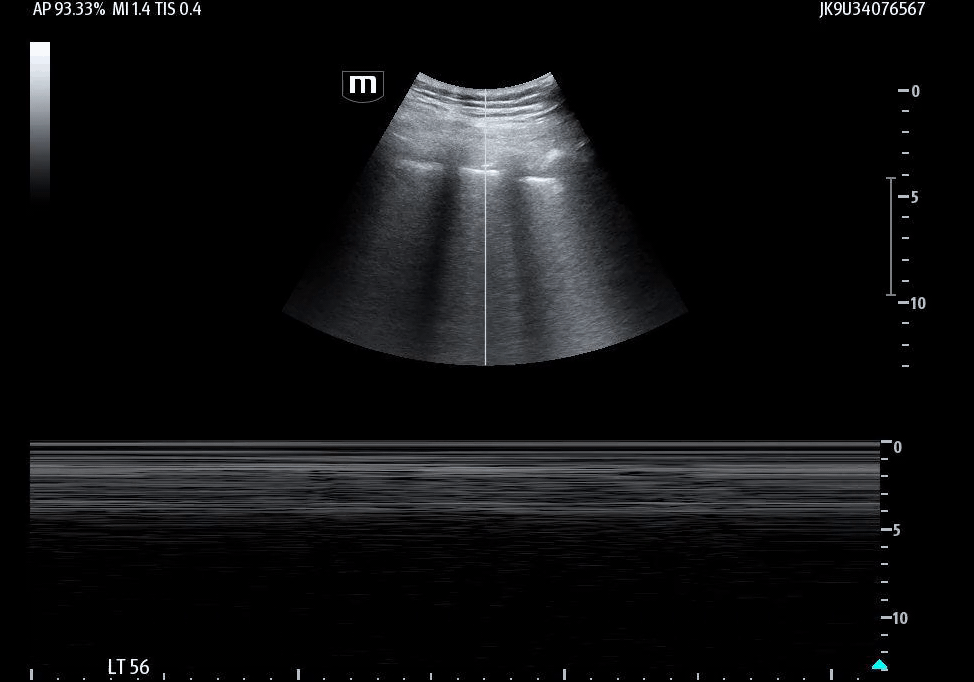
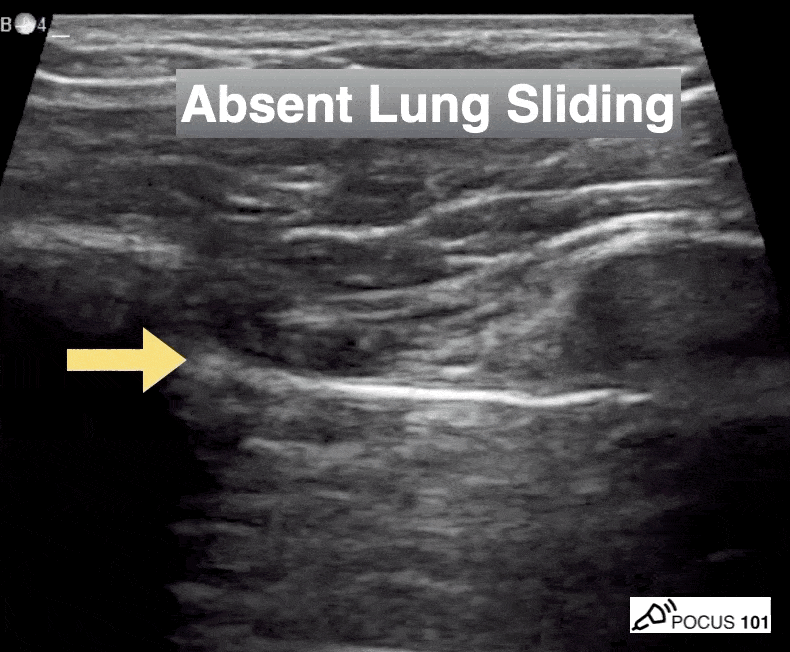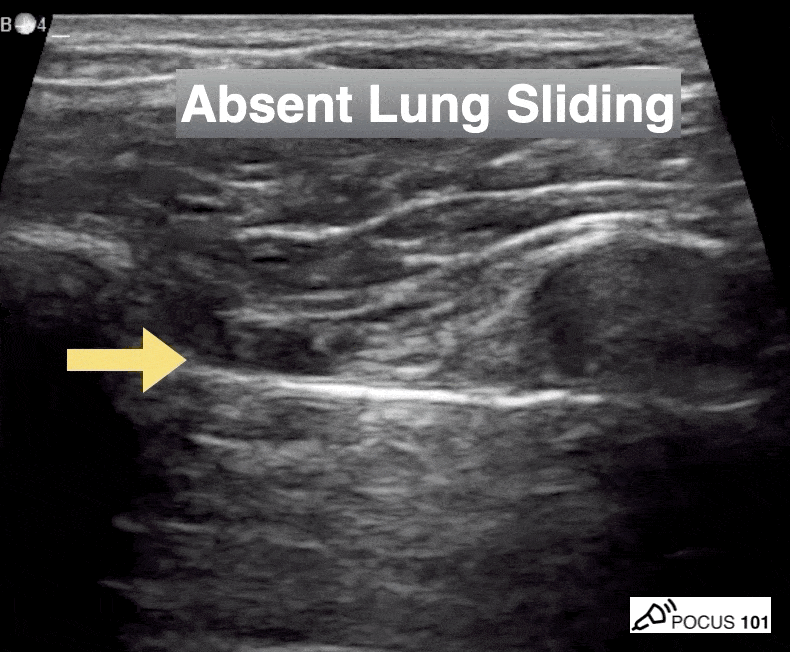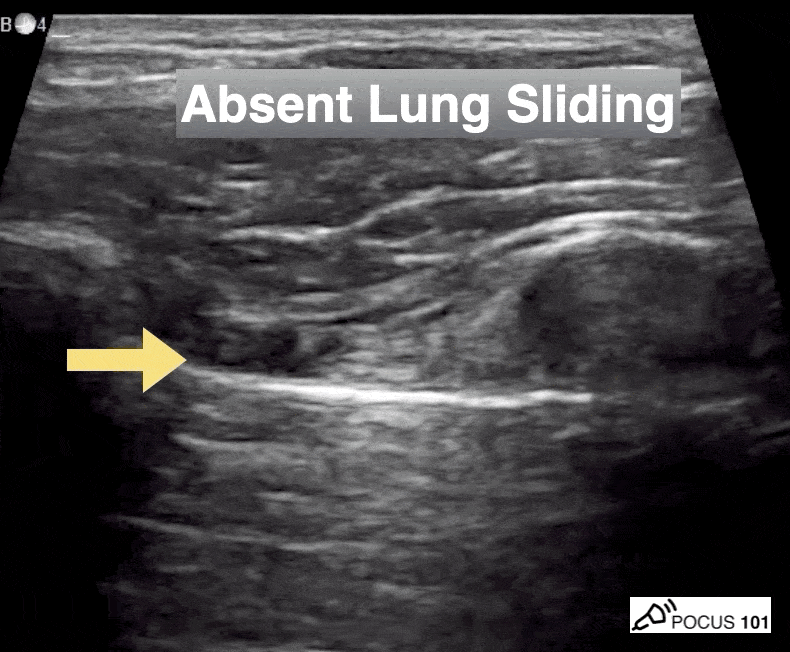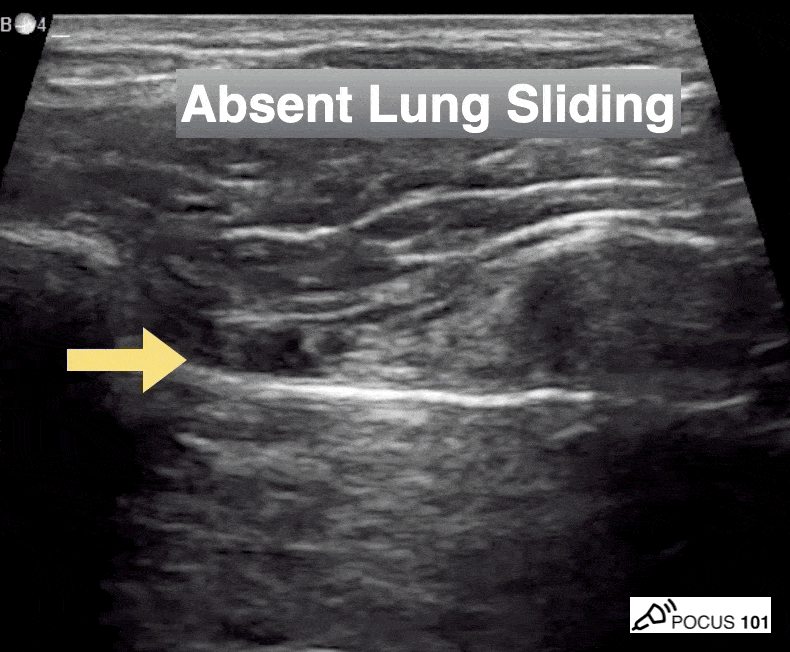
She isn’t crashing—but she isn’t stable either. Luckily, an ultrasound is immediately available. An eFAST exam is performed, revealing the following:
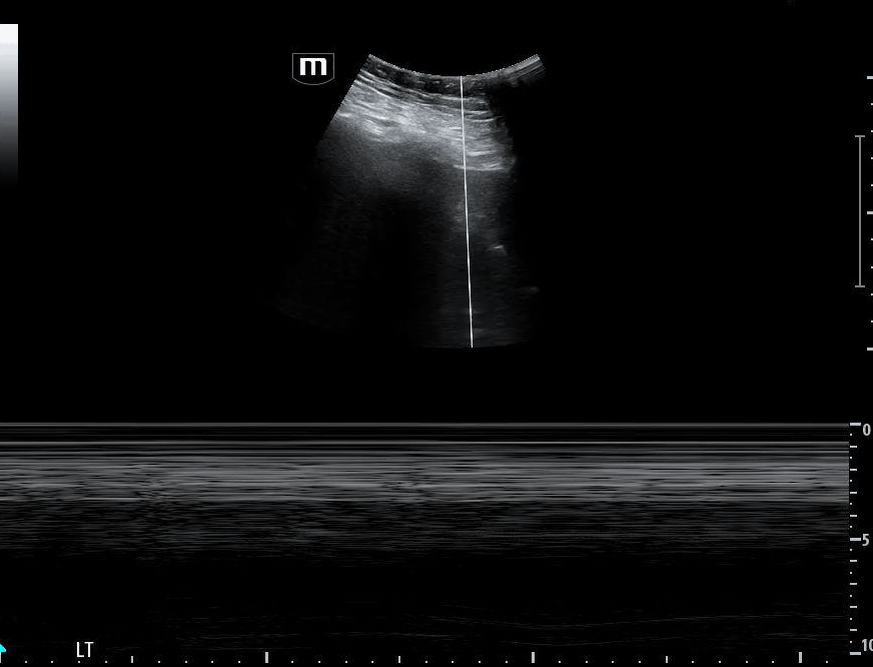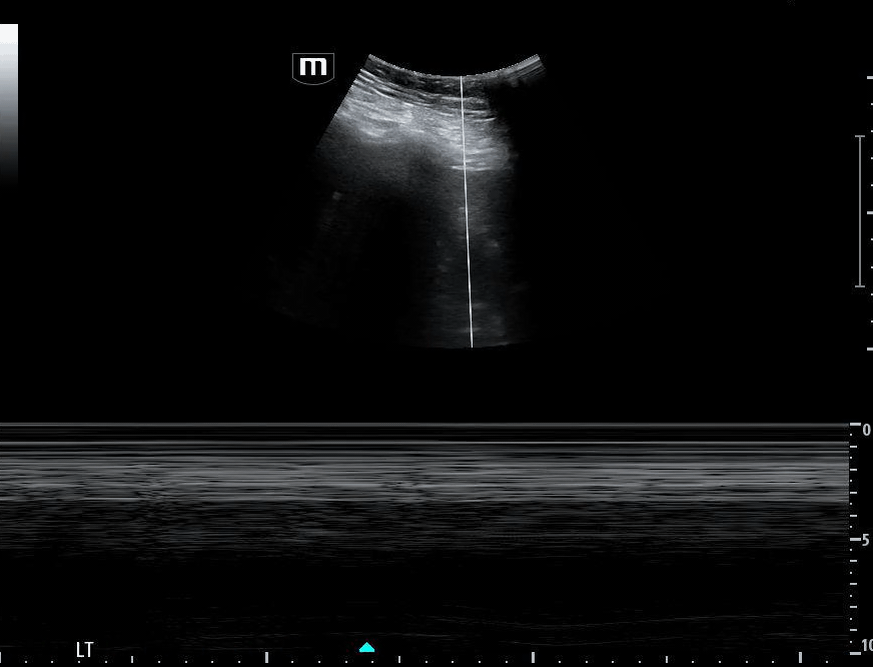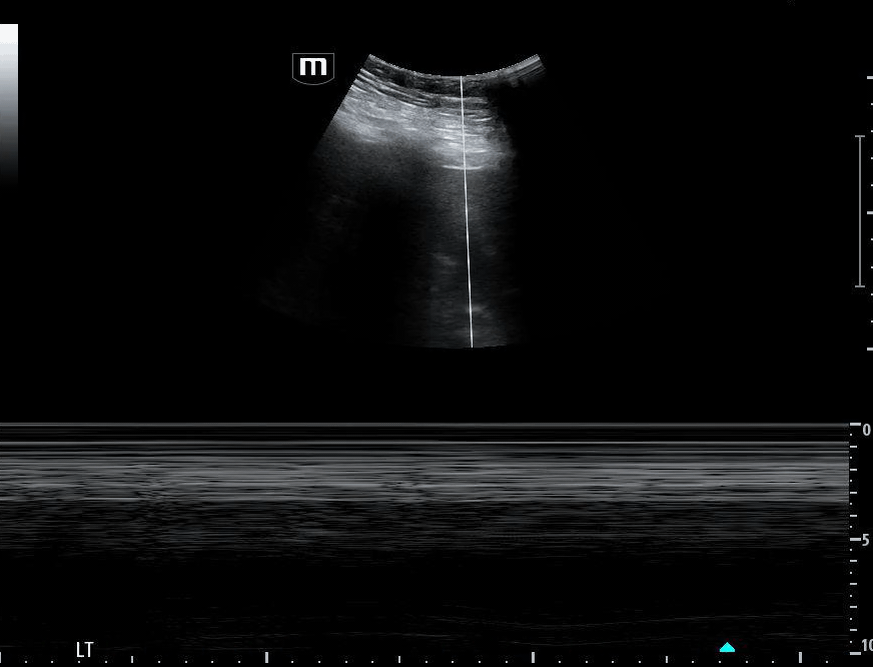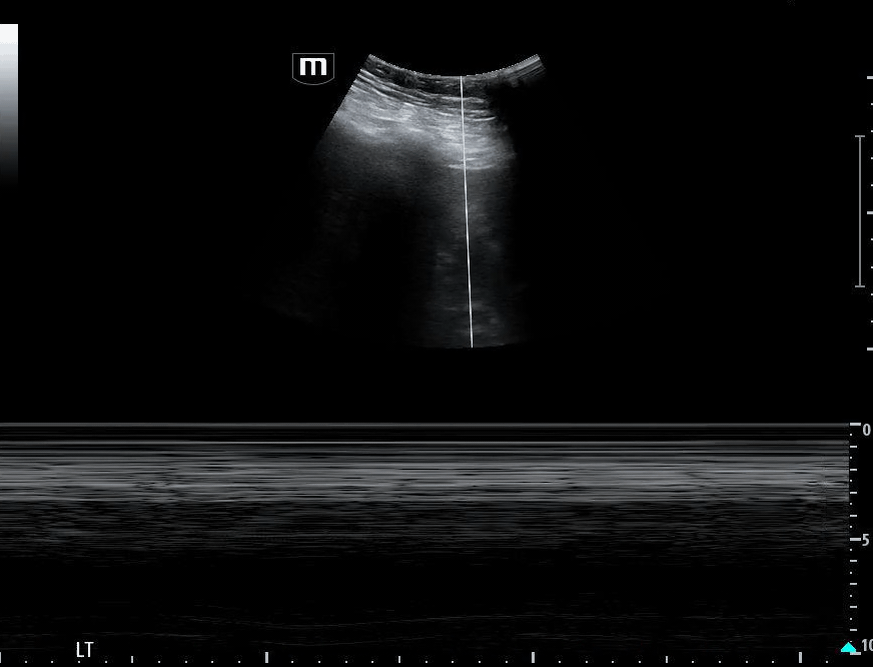
Image 1 demonstrates the left lung view with absence of lung sliding.
Image 2 confirms this finding using M-mode, demonstrating the classic barcode sign, which is consistent with absent pleural motion.
Now comes the critical decision point: Do you place the chest tube now? Do you wait for confirmatory imaging? Or do you gather more ultrasound information before committing to an invasive procedure?
Additional ultrasound imaging are obtained:
Image 3 demonstrates the expected location of the parasternal long-axis (PSL) view; however, the PSL view is notably absent at the left sternal border.
Image 4 instead reveals cardiac activity visualized to the right of the sternal border, suggesting mediastinal shift.
Image 5 shows a subxiphoid cardiac view
Image 6 demonstrates a plethoric inferior vena cava (IVC), concerning for elevated intrathoracic pressure and impaired venous return.
A chest tube is placed in the left thorax due to concern for tension pneumothorax. The team prepares for the expected rush of blood consistent with hemothorax. Instead, yellow pleural fluid begins to drain. More fluid continues to collect in the chamber. By the time the initial drainage slows, a total of 3 liters has been evacuated. But something else is concerning—the pleuravac reveals a persistent air leak.
Shortly afterward, the patient’s clinical status begins to change. Her oxygen requirements increase. She develops a persistent cough and complains of worsening shortness of breath.
Repeat ultrasound and chest radiography are obtained, showing the following:
Image 7 demonstrates the return of lung sliding following chest tube placement, indicating reexpansion of the lung and restoration of pleural apposition.
Image 8 confirms this finding on M-mode, showing the classic seashore sign, which is consistent with normal pleural motion.
Interval imaging in Image 9 reveals the presence of multiple B-lines in more than two lung fields, concerning for pulmonary edema and consistent with reexpansion pulmonary edema in the appropriate clinical context.
So what happened to this patient and how can we use ultrasound to guide our management?
Point-of-care ultrasound (POCUS) is fast, repeatable, and often more sensitive than chest radiography—especially in supine patients.
Overall, lung ultrasound demonstrates a sensitivity of approximately 77–91% and specificity of 98–99% for pneumothorax.
Absent lung sliding
Highly sensitive (approaching 100% sensitivity); Less specific (~78% specificity)
Important limitation: absent lung sliding is not unique to pneumothorax; may also be seen in:
Atelectasis
Consolidation
Pulmonary contusion
Mainstem bronchial obstruction
Pleural adhesions
Because of this, absent lung sliding alone cannot definitively diagnose pneumothorax. The following findings increase the specificity and therefore provide a more definitive diagnosis.
Absent B-lines
Significantly improves specificity to 94–98%
B-lines require visceral and parietal pleural contact, so their absence increases concern for pleural separation
Presence of Lung point
This finding is 100% specific for pneumothorax
The lung point represents the exact boundary between collapsed and aerated lung
Absent lung pulse
Its absence further supports pneumothorax and increases diagnostic specificity
The lung pulse reflects transmission of cardiac activity through an intact pleural interface
Furthermore, ultrasound can also identify early signs of tension physiology—even before classic vital sign abnormalities develop.
Suspicion for evolving tension pneumothorax should increase if ultrasound shows:
Mediastinal shift
A plethoric, non-collapsing inferior vena cava (IVC)
Management: Does Every Pneumothorax Need a Chest Tube?
Not all pneumothoraces require urgent interventions. Indications for urgent chest tube placement include:
Tension pneumothorax: Defined by pneumothorax plus clinical signs of physiologic compromise, such as
Hemodynamic instability
Respiratory distress
Tracheal deviation
Jugular venous distension
Cyanosis
Hemodynamic instability in the presence of pneumothorax
Large pneumothorax
Greater than 2–3 cm from lung margin to chest wall
Greater than 20% of thoracic volume
If none of the above criteria are met, observation with supplemental oxygen and serial reassessment may be appropriate, typically for at least 24 hours.
Ultrasound is especially valuable here, allowing real-time monitoring without repeated radiation exposure.
Regional anesthesia is an underutilized but highly effective adjunct that improves patient experience and may reduce opioid requirements. Consider before or after placement of a chest tube. In our patient, an erector spinae plane block was performed prior to chest tube placement. Pain improved dramatically—from 7/10 to 1/10 following the block.
Important Chest Tube Management Principles
When placing a chest tube, caution should be taken to avoid rapid expansion.
For fluid drainage (pleural effusion):
Avoid draining more than 1,500 mL initially
For hemothorax, surgical surgical intervention is needed if:
Immediate drainage >1,500 mL
Ongoing drainage >200 mL/hour for 2 hours
For air leak (pneumothorax) + fluid draining (pleural effusion):
Allow fluid drainage >1,500mL
Avoid clamping to decrease changes of tension pneumothorax
Monitor closely for complications of rapid expansion
A Rare but Serious Complication: Reexpansion Pulmonary Edema
Reexpansion pulmonary edema is an uncommon but potentially life-threatening complication that occurs after rapid reexpansion of a chronically collapsed lung. Risk factors include:
Lung collapse for greater than 3 days
Rapid drainage of large volumes (>1–1.5 liters)
Younger age
Application of negative pressure suction
Clinical presentation may include:
Dyspnea
Persistent cough
Chest discomfort
In severe cases, this can progress to respiratory failure and hemodynamic instability.
Imaging with ultrasound or chest radiography typically shows findings consistent with pulmonary edema.
Treatment is supportive and may include:
Supplemental oxygen
Careful respiratory monitoring
Diuretics in select patients
Escalation to mechanical ventilation if needed
In this patient, ultrasound rapidly identified absent lung sliding and evolving tension physiology, prompting timely chest tube placement.
Ultrasound continued to guide care after intervention by confirming lung reexpansion and allowing early recognition of reexpansion pulmonary edema.
Pneumothorax management does not end with tube placement; it requires ongoing reassessment, thoughtful drainage, and vigilance for complications.
By integrating ultrasound at every stage from diagnosis, to intervention, to monitoring; we can make faster, safer, and more informed decisions at the bedside.
In the trauma bay, seconds matter, and ultrasound allows us to see pathology unfold in real time, often before the patient declares it clinically.
Happy scanning!
References:
Dinh V, Deschamps J, Ahn J, et al. Lung ultrasound made easy: step-by-step guide. POCUS 101. Published online 2023. Accessed February 18, 2026.
Alrajhi K, Woo MY, Vaillancourt C. Test characteristics of ultrasonography for the detection of pneumothorax: a systematic review and meta-analysis. Chest. 2012;141(3):703–708. doi:10.1378/chest.11-0131
Inocencio M, Childs J, Chilstrom ML, Berona K. Ultrasound findings in tension pneumothorax: a case report. J Emerg Med. 2017;52(6):e253–e256. doi:10.1016/j.jemermed.2017.01.035
Cusumano G, La Via L, Terminella A, Sorbello M. Re-expansion pulmonary edema as a life-threatening complication in massive, long-standing pneumothorax: a case series and literature review. J Clin Med. 2024;13(2):XXX. doi:10.3390/jcm1302XXXX
(Note: replace XXX with final page/article number if needed depending on journal formatting)
Baumann MH, Strange C, Heffner JE, et al. Management of spontaneous pneumothorax: an American College of Chest Physicians Delphi consensus statement. Chest. 2001;119(2):590–602. doi:10.1378/chest.119.2.590